Anal Fissure Treatment In Kolkata
If you’ve ever felt like you’re ‘passing shards of glass’ during a bowel movement, you’re not alone—and you don’t have to suffer in silence. For effective anal fissure treatment in Kolkata, Proctosafe Clinic offers expert care combining Ayurvedic wisdom with modern surgical precision for lasting relief.
What is an Anal Fissure?
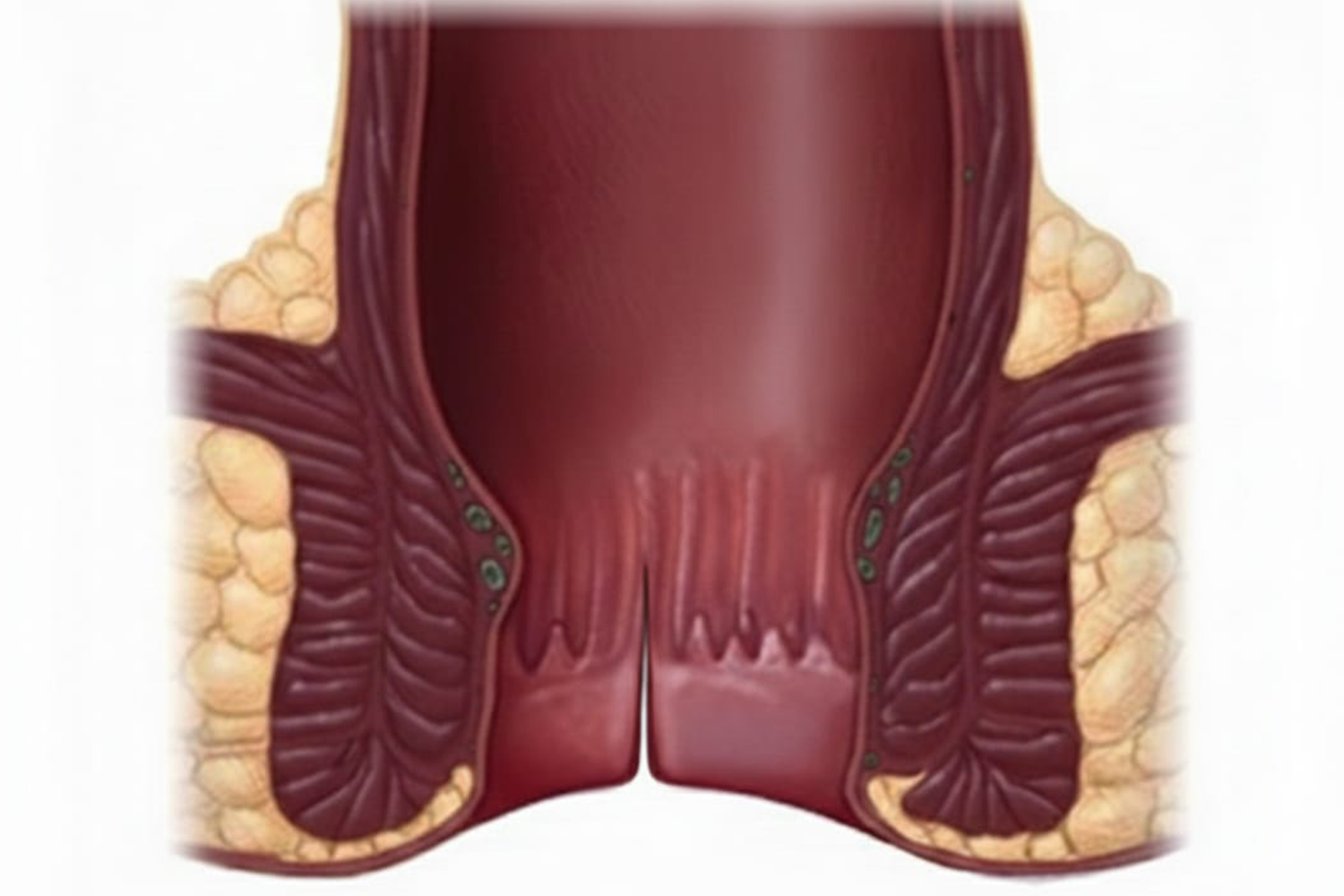
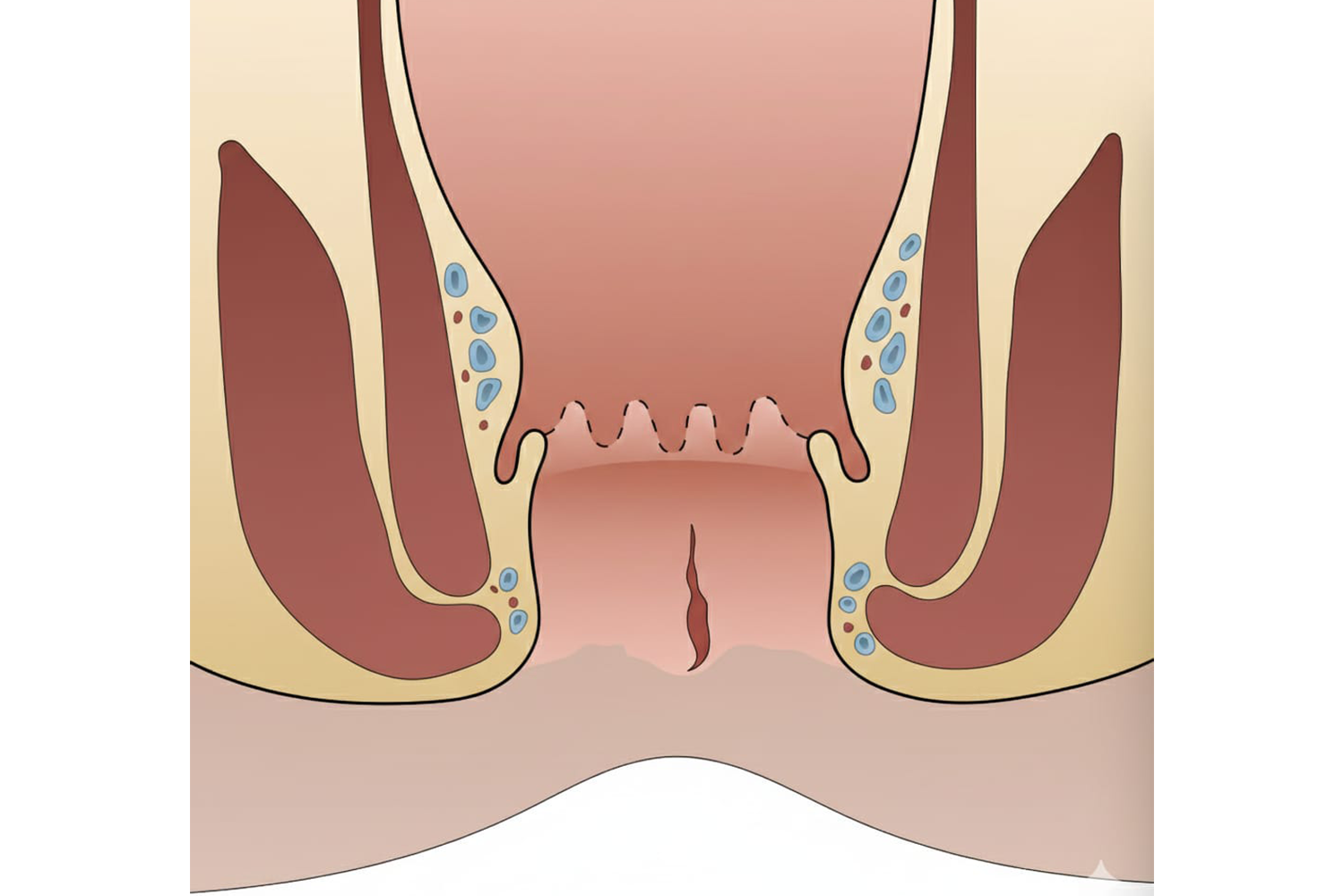
An anal fissure is a small, linear tear or crack in the moist, thin tissue (mucosa) that lines the anus. More specifically, it occurs at the junction of skin and mucous membrana of anal orifice.
Pathogenesis: The Vicious Cycle
How does a tiny tear cause so much trouble? It follows a specific pathological path:
- The Trigger: Most commonly, a hard stool or chronic diarrhea causes an initial tear in the anoderm.
- The Spasm: The exposed internal anal sphincter muscle goes into a painful spasm to protect the area.
- Reduced Blood Flow: This spasm compresses local blood vessels, reducing blood supply (ischemia) to the wound.
- Non-Healing: Without adequate blood flow, the fissure cannot heal naturally, leading to a chronic, painful ulcer.
What Causes Fissure?
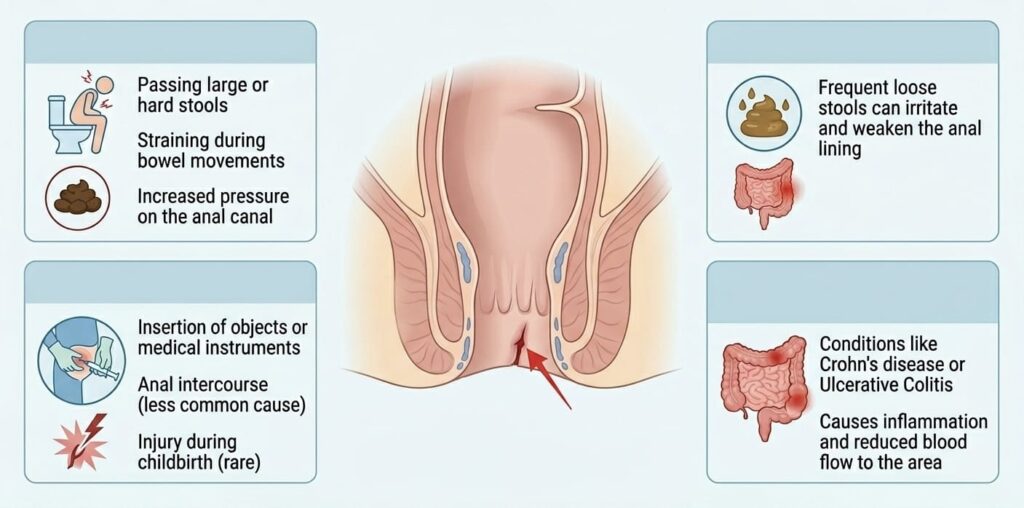
While constipation is the usual suspect, several factors can lead to a fissure:
- Chronic Constipation: Straining to pass hard, dry stools.
- Diarrhea: Frequent, irritating bowel movements.
- Childbirth: Trauma to the anal canal during labor.
- Inflammatory Bowel Disease (IBD): Conditions like Crohn’s disease.
- Tight Sphincter Muscles: High resting anal pressure.
Modern Office Syndrome: Long sitting position compromises blood flow to the bottom.
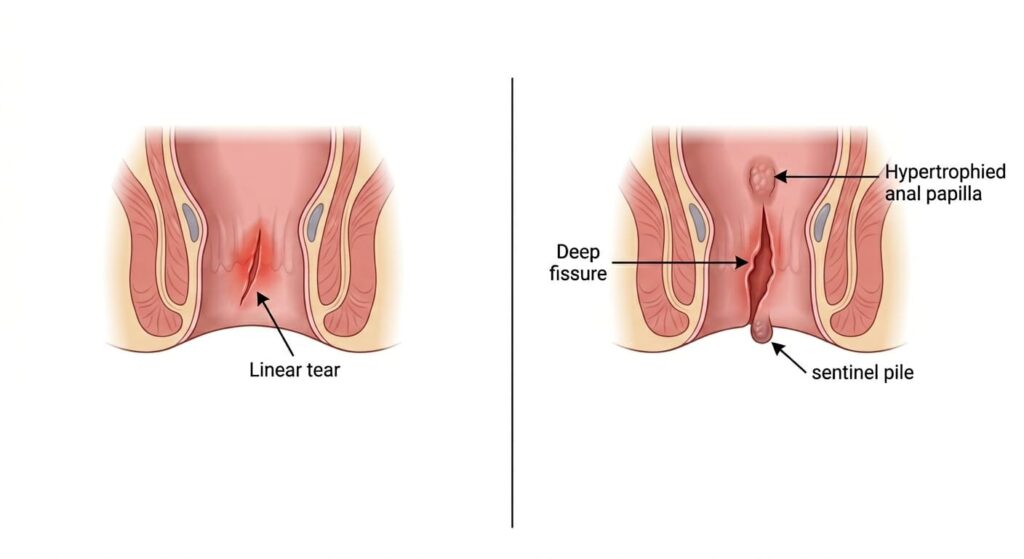
Types of Anal Fissures
Acute Fissure: Less than 6 weeks. Looks like a fresh tear; usually heals with conservative medical management.
Chronic Fissure: More than 6 weeks. Deep tear often accompanied by a “sentinel pile” (skin tag) or hypertrophied papilla. Requires surgical intervention.
Diagnosis: How will you know?
At Proctosafe Clinic, diagnosis is primarily clinical. Our experts perform a gentle visual inspection. In most cases, a digital rectal exam (DRE) is avoided in the acute phase to prevent unnecessary pain. For chronic cases, we may use a Proctoscope to assess the depth and state of the internal sphincter. In doubtful conditions, colonoscopy is done.


The Proctosafe Clinic Advantage: Ayurvedic Speciality
Led by our specialist Ayurvedic Surgeon, we provide tailored medical and surgical solutions. For early-stage cases, we utilize safe and potent Ayurvedic formulations that facilitate complete recovery within a short timeframe. For chronic fissures accompanied by sentinel tags, our surgeon performs minimally invasive procedures designed for lasting relief and a rapid return to daily life.
